It’s been four days since my second brain surgery. I’m still in the post brain surgery fog, yet felt compelled to write about my experience so far. I’m grateful for those of you following along in this season, knowing my story could help just one person advocate for themselves medically, fills my heart.
The morning of surgery was exceptionally rainy with flooded roads and as I drove us to the hospital at 6:15 am I couldn’t help but think about how much the journey to the hospital paralleled this aneurysm journey so far. It was a slow, dark, cautious trek, with lots of unknowns and many slow downs.
I got checked in right away and taken back to the procedural waiting room. I felt calm and ready. I felt very strongly we were supposed to do this surgery and I was grateful Dr. M and his team worked with my teaching schedule to get it done as soon as my break started.
I texted my people as I waited for the procedure to begin, feeling steadfast and nervous, the continuous coexistence of this season. I knew I had to have an iv put in, my wrist prepped and to speak to Dr. M and his team before they would bring me back. Dr. M, in his usual gentle giant presence told me he had all the confidence things would go quickly and easily and he was hopeful to not see the left sided aneurysms when he went in. He reminded me that I would not wake up with a bloody scalp like last time (and commended me again for being his change agent in changing how neuro-monitoring is done for his surgeries!) As soon as my wrist was prepped, I texted my people again and made sure they all knew how much I loved them. I was ready to begin the exit strategy for aneurysms 3 & 4!
Going into the procedure room is a bit daunting, there’s a large screen that projects many, many different images of your brain from previous scans on the wall as you enter. There are also a lot of doctors and nurses in the room, it’s a flurry of activity and I will admit I had a deeply emotional moment realizing they were all there to save my life, for the second time. It’s humbling for sure.
I’ve always been someone who does not take to getting IV’s well, and this procedure was no different. As the anesthesiologist was trying to get the anesthesia in he encountered some resistance from my vein. His wonderful nurse, who had the oxygen mask over my nose and mouth leaned in close when she saw my panic (because it wasn’t working at first) and spoke calmly and reassuringly to me. Finally, it worked and I was asleep.
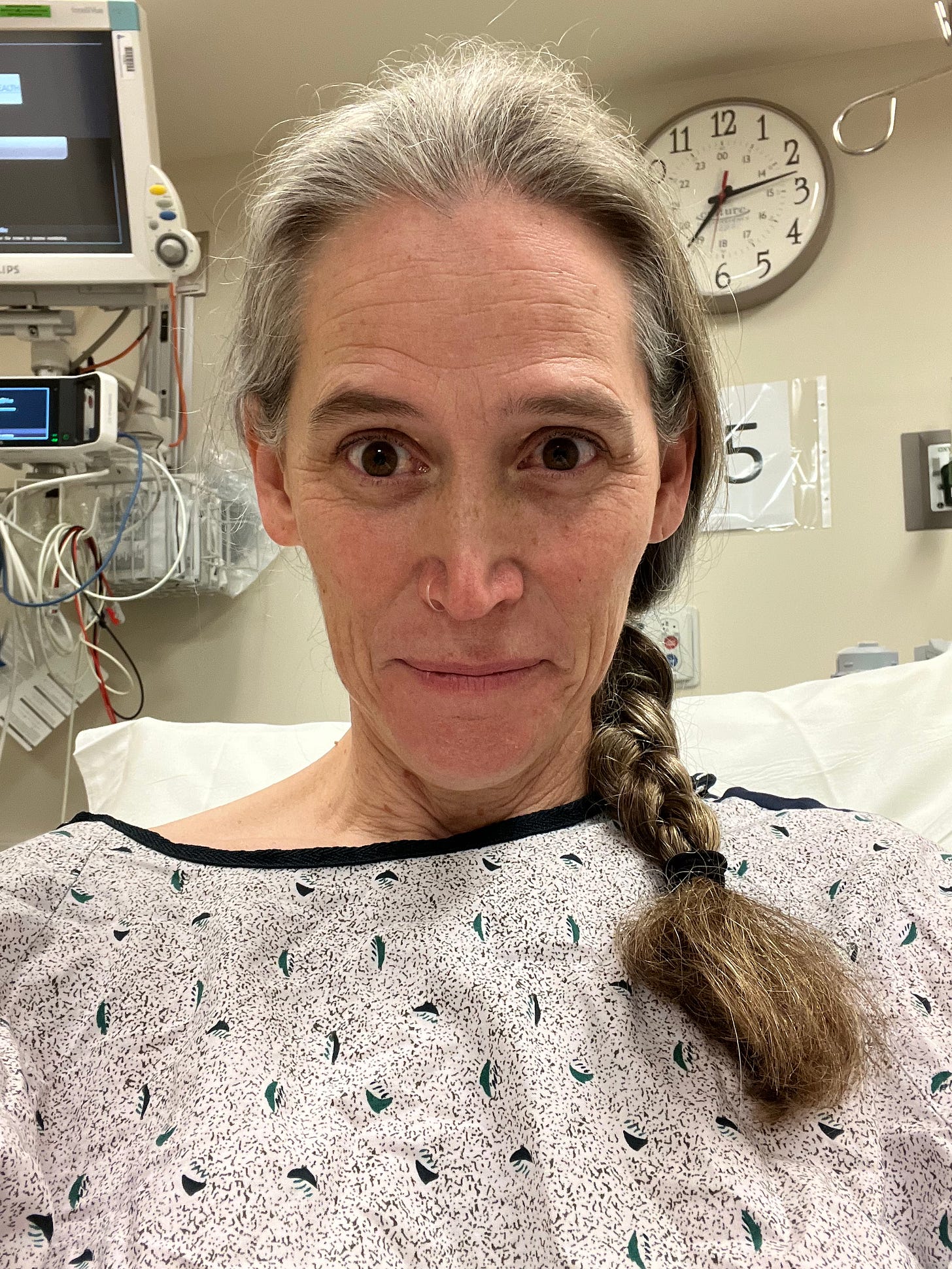
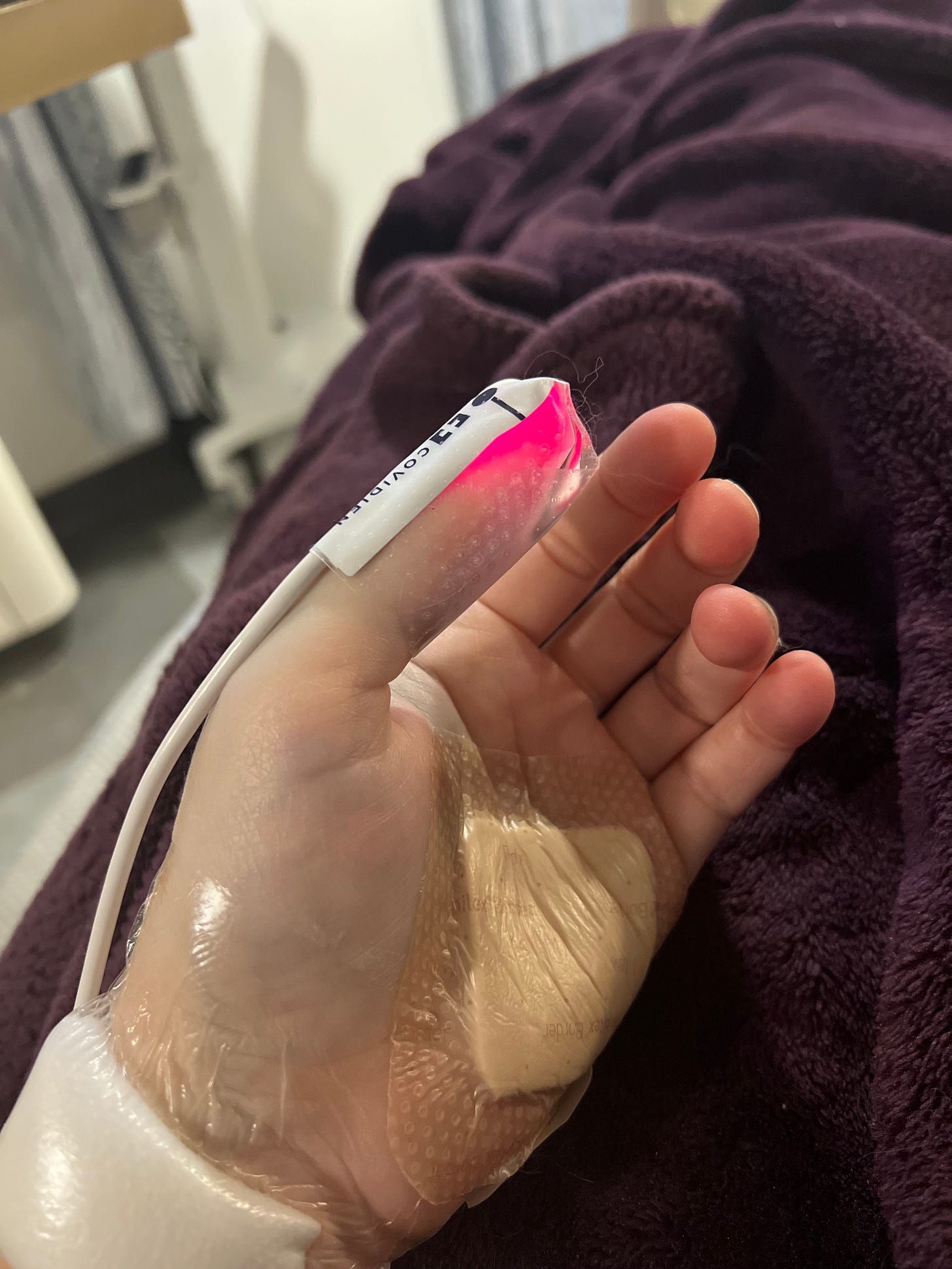
I woke up in the ICU about 4.5 hours later and distinctly remember noticing that this surgery took longer than the last one did. I made a mental note to ask my people if I was right. The two nurses caring for me in the ICU were wonderful, as it’s unnerving to fall asleep with one IV in your arm and wake up to three iv’s, a catheter inserted and a pressure bracelet over your surgery site in your wrist! Instantly I told them something didn’t feel right with my arterial IV in my left wrist, it hurt something awful and my hand was already beginning to swell. I also had a wound on my hand that wouldn’t stop oozing blood (no one knows how I got it). However, I was so grateful to not wake up to an oozing bloody head this time!
My nurses also noticed how quickly my hand was beginning to swell and put in a call to Dr. M’s PA to inquire about what may be happening. It was determined blood had backed up into the arterial line and was causing the pain and swelling and they decided to remove it (it’s usually left in to monitor blood pressure for 24 hours because of high risk of stroke). Taking it out took away some of the pain, but it was still really uncomfortable and I couldn’t move my fingers very well. The swelling got worse over night, so much so that I asked them to move my blood pressure cuff to my other arm because it was causing unbelievable pain each time it inflated. They typically don’t put the cuff on the surgery site arm, but felt this was the best option given the level of swelling in my hand (at that point during the night I couldn’t move any of my fingers).
For the first 24 hours post surgery, they monitor you very often, assessing strength and feeling, especially on the side of the body that would be affected by the surgery. For this surgery it was my left side of my body, so they were very mindful of what was happening with my hand. Both nurses recognized decreased strength in my left hand, but felt it would be because of the swelling. Though as time went on my left leg began to feel too heavy to lift and I had tingling on the left side of my face. Dr. M came in to assess and he said his gut instinct was after affects of the anesthesia, but he wanted to do a cat scan to be sure. He also told me that he jinxed himself by saying it would be a smooth easy surgery, in fact he said it was very tough to access the aneurysms and it took a lot longer than he anticipated. I’m anxious to learn more about that in my follow up appointment with him. He was elated to report to me that he could NOT SEE the two left sided aneurysms at ALL when he was in my brain and he couldn’t wait to show me the images! That made us all happy.
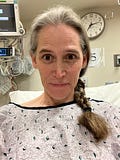
Down in the CT room, once again my IV site would not cooperate and it took the nurses and CT tech 4 tries to get a new IV in my right arm. I told the wonderful women trying to get my veins to cooperate it was like a bad breakup saying “Ladies, it’s not you, I swear, it’s me!” They laughed yet I know they felt awful for sticking me so many times. Luckily, the CT scan came back clean and it was determined my weakness issues were related to the anesthesia. My people and I were so grateful for those results. Our daughter combed out my sticky hair for me and popped it up into a bun so I could sleep easier, it made me feel human!
The next morning I woke up with a horrible migraine, to the point I was nauseated, and sweating profusely, so they needed to give me medication so I wouldn’t begin to vomit (very bad thing to happen post brain surgery!) and a migraine cocktail. Dr. M came in to tell me he wanted me to be seen by the PT and stay another night because of the weakness and the intensity of my pain. He also wanted to start me on a round of steroids for the pain. I was sad, yet also relieved, because I wanted to be sure I felt steady enough to go home to my people. I felt really awful that morning.
Thankfully, I was finally able to go home the next morning, as I woke up feeling much better and was anxious for my bed, my cats and my people!
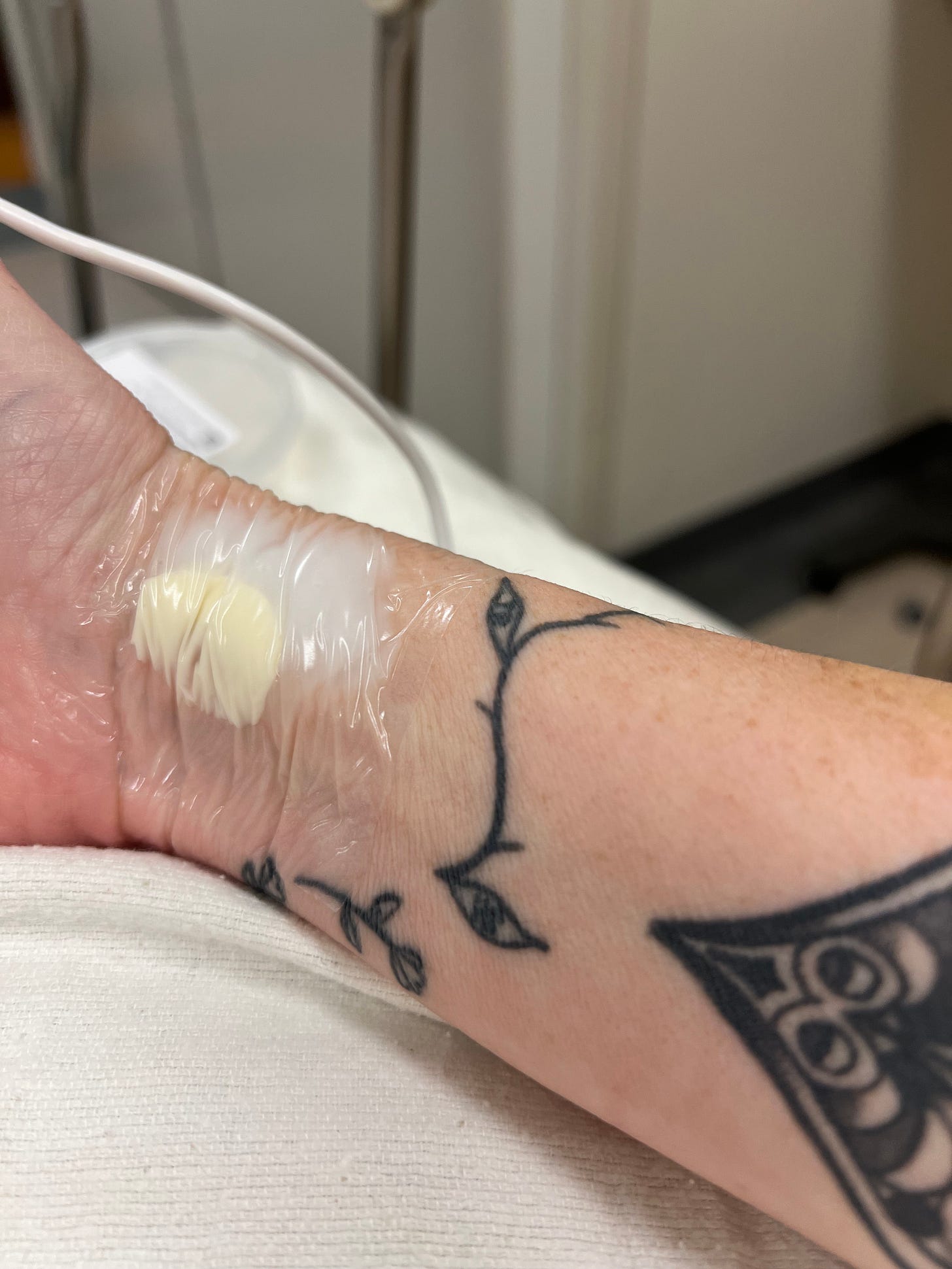
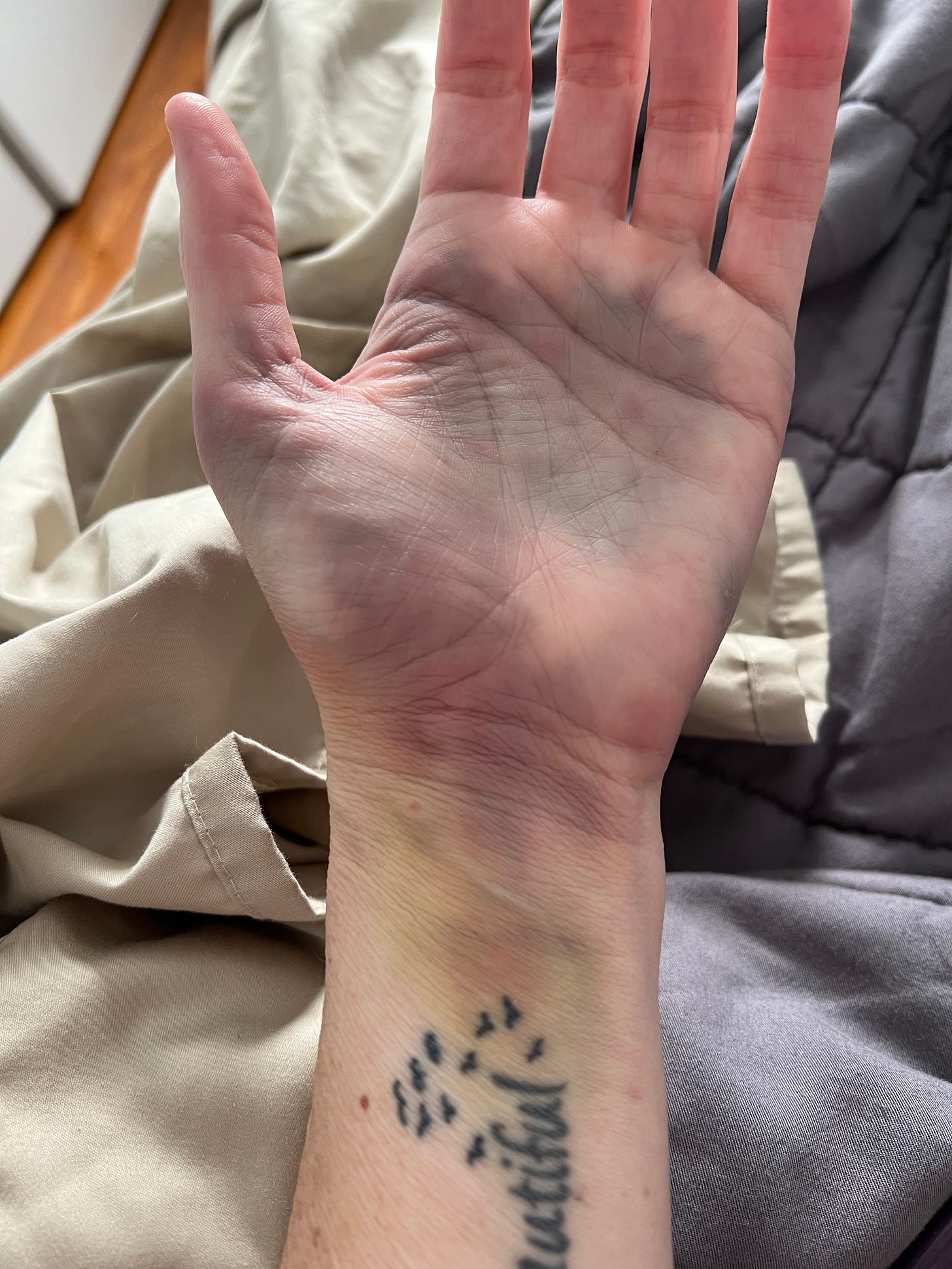
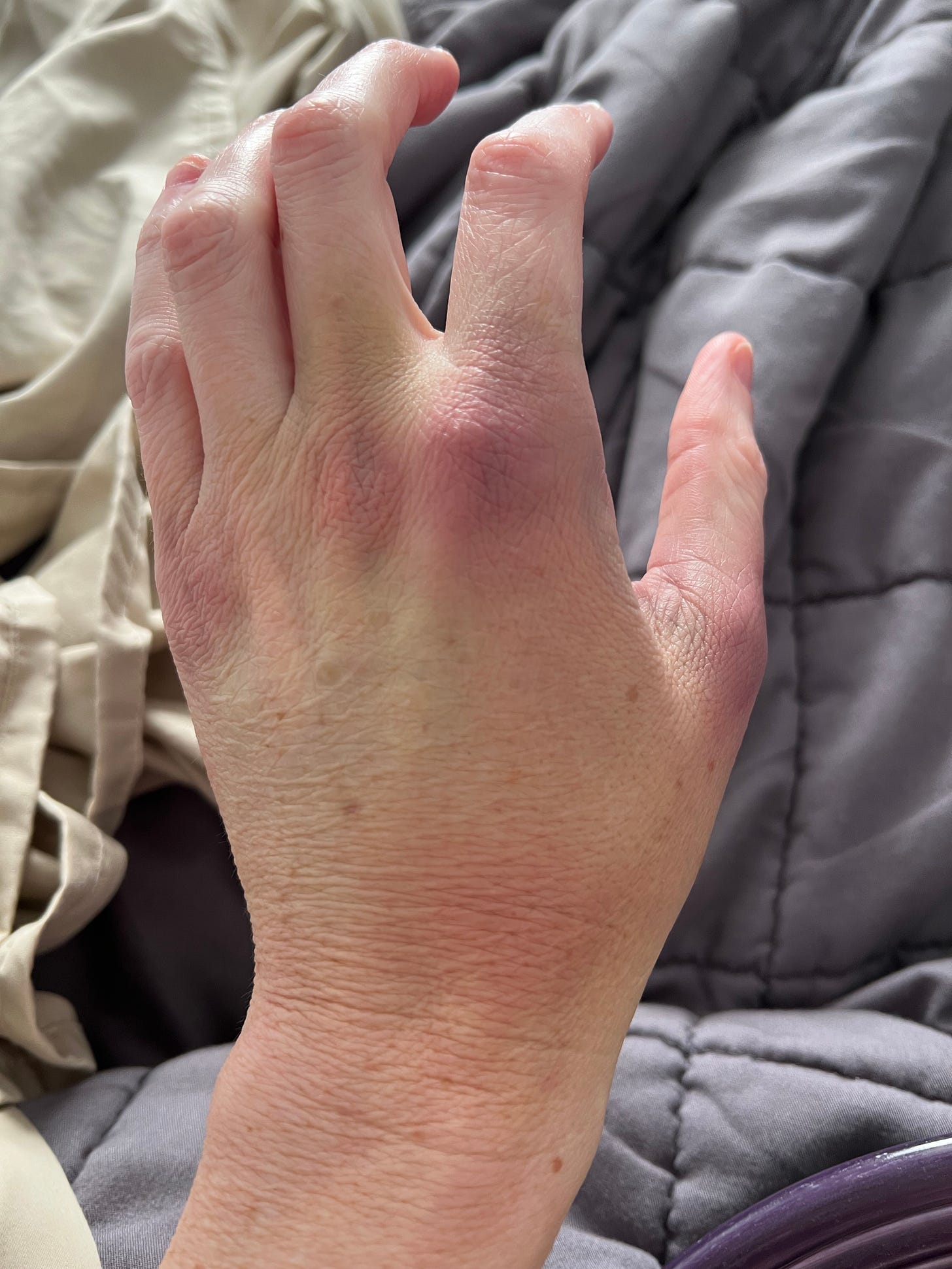
As more my IV’s came out and the bruising began to appear. As a person on blood thinners, my level of bruising is intense, and continues to surprise me! I took these photos of my bruises from my arterial line after coming home. I keep telling people I look like I got into a fist fight with the anesthesiologist! My surgery site is bruised and causing pain, but doesn't look as wicked as my left hand.
This recovery has been very different than my first one, a harder ride emotionally, and filled with more pain, yet it’s also been a bit easier because I knew what was coming. I’m still filled with brain fog, my arms both hurt a lot and I’m still suffering from headaches. I’m also filled with gratitude and humility for all that happened to get me (and my people) to this point. I’m anxious for my follow up yet fully trust Dr. M and his team.
To all of you who have prayed for me, held space and sent me well wishes, my gratitude continues to be immense. I can feel all of it and it’s carrying me through!
Warmly,
Jane



Such great details (especially for someone who has brain fog ). Praying the rest of your recovery goes well.